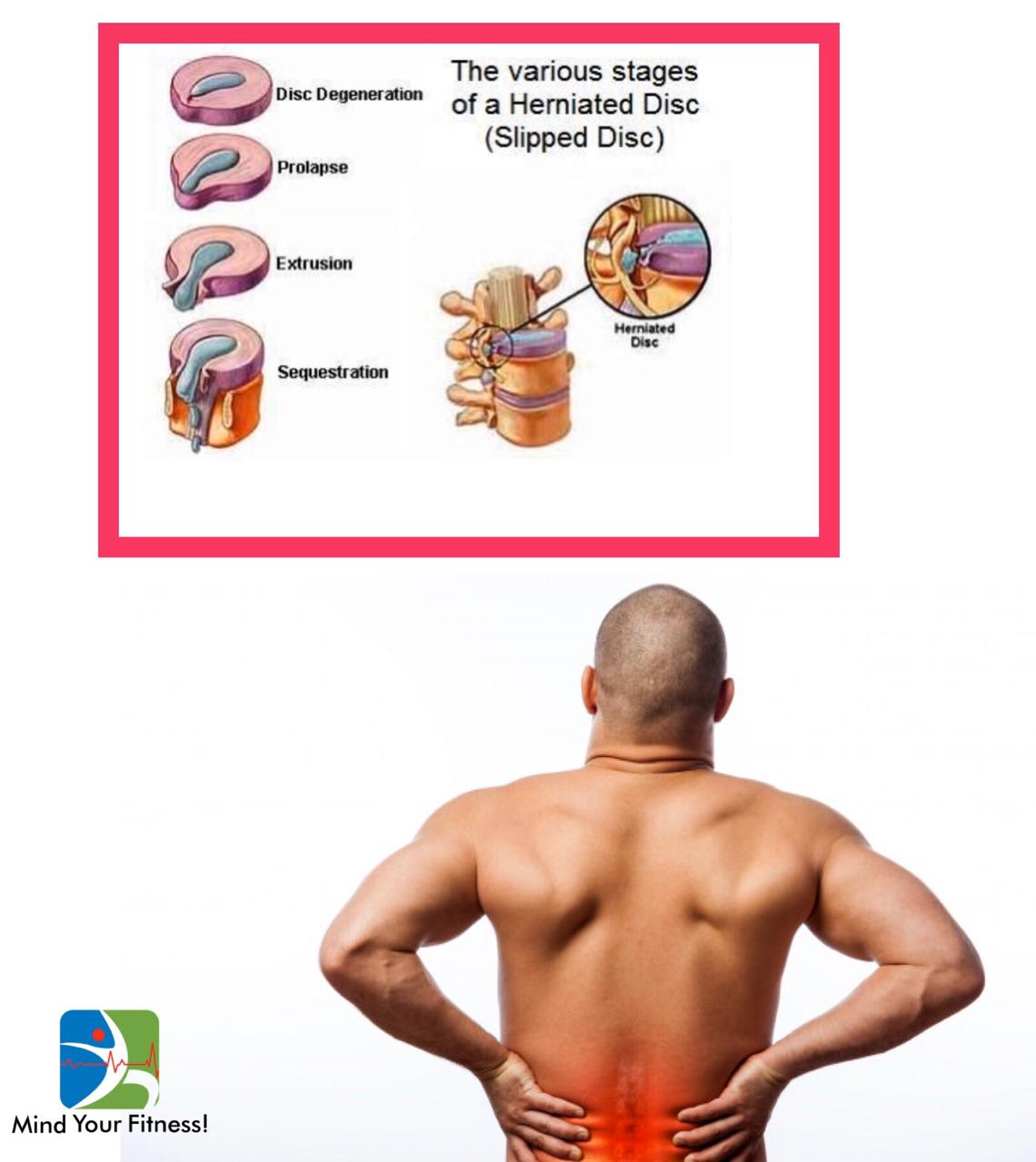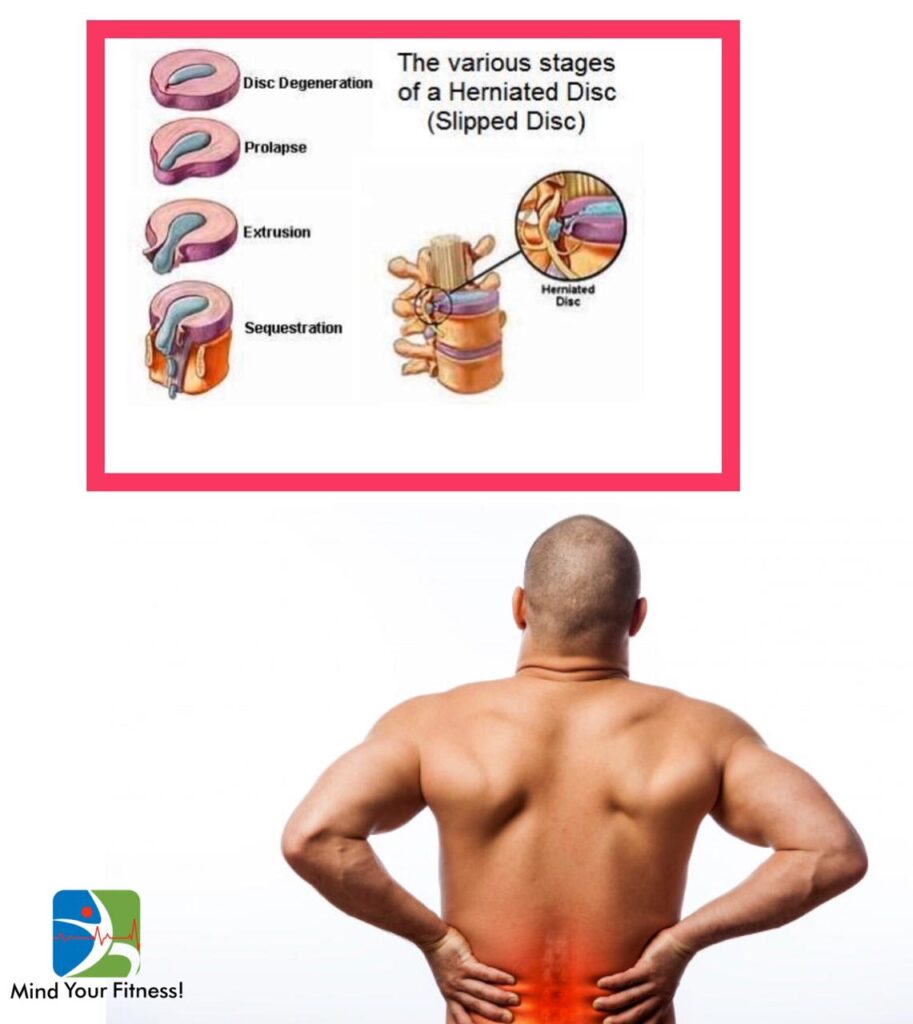
What is PIVD?
-It is known as the prolapse of the intervertebral disc and is commonly known as “slipped disc” or “herniated disc”.
Discs are cushion-like structures between the vertebrae of the spine which help in shock absorption, in absorbing the shear forces placed on the spine in antigravity movements like standing, sitting, walking or running.
The disc slips due to excessive pressure on it thereby bulging out of place in either frontwards or backwards direction from its position, putting added pressure on the spinal cord or any single nerve fibre.
The causes of low back pain can vary. It can happen during one dubious repetition while lifting in a gym or simply while bending forward to pick up a child or due to prolonged sedentary lifestyle-induced sitting posture.
Common myths:
As soon as you are diagnosed with a bulging disc, many may get the advice to do complete bed rest and avoiding any kind of activity or exercises even when the first acute phase of the back pain has settled or if you are only left with mild dull aching pain around the back often leading to fear of not moving/straining the back again.
Investigations:
Common terminology used to patients by the doctor after an X-Ray and MRI are:
- the disc is bulging out
- there is a trapped nerve
And in either of the cases above, there is an MRI to prove it.
The intervertebral disc thereby becomes a sole reason for a lot of back pain and disability related to it, often bypassing other problems like any core and back muscle weakness, bad posture, poor spinal alignment and deviation in its natural spinal curves, heredity of back pains, alimentary system dysfunction, kidney dysfunction (inflamed visceral organs gimmick low back pain sometimes), limb length discrepancy etc.
The use of the term “disc” tends to create a cascade of fear, anxiety and worry in the patients for their future and overall health, without understanding that wear and tear is inevitable but recovery and programming the brain to treat the symptoms with core and back muscle strengthening is a necessary “choice”.
How can slipped discs be prevented?
The answer is subjective to each person. PIVD can happen without any prior prediction but with a proper exercise routine to strengthen the posterior chain muscle groups (the hamstring muscles, the hip muscles, the muscles of the back) and the abdominal muscles can prove useful for better spinal health and integrity.
This brings us to two main questions:
1) Are herniated discs bad/life-threatening?
No.
Herniated disc is not necessarily a bad prognosis.
One the acute phase of the back pain kicks in, the possibility of a muscle spasm is there as a body’s normal response to excessive strain on the spine. This can hamper walking or sitting or moving from anywhere between 3-7 days. In certain cases, complete bed rest with a course of anti-inflammatory drugs may be advised. Age also plays a vital role.
Not all disc herniations guarantee severe back pain symptoms.
Disc herniations can exist in pain-free people too.
The older we get, there is a likely chance to find more signs on MRI but a person may not necessarily have low back pain.
How do you know if the MRI findings are legit?
- Pathology of back pain varies.
- the MRI can be referred for understanding the key points of back pain. If the assessment by the physiotherapist matches the symptoms and findings in the MRI reports, there is an active wound or manifestation of back pain and can be treated accordingly. If the correlation of symptoms does not match with the MRI findings, then the back pain situation isn’t grave.
2) Will exercising lead to increased risk or injury to the spine in the future?
NO.
Exercises can be done incrementally, under the guidance of the physiotherapist as per the current symptoms and then increased for further strengthening of the vulnerable muscles. The dose of exercise will vary from person to person.
The spine is designed naturally to undertake shear forces and compression forces depending on the load put on it. Postural assessment and postural screening while a patient performs various weight lifting techniques can be done in order to help the spine remain injury-free or prevent further injury.
- Letting the discs adapt to the added load via weights, initially starting with low-intensity workouts, because discs will adapt due to natural healing responses of the body. If we stop exercising due to back pain, the body loses the level of fitness and its sense of adaptation to loads, rendering the muscles weak.
- One should not add weights too soon to avoid flare-ups.
- the assessment predicts the amount of recovery time from that back pain. Sedentary lifestyle individuals and non-exercising people can benefit from isometric or static home exercises as well as mild resistance thera-band exercises initially before progressing to other exercises.
The previous history of any surgery or major injury to the spine can contribute to the recovery time. A longer time of recovery is permissive so that the spine recovers fully to its optimal function.
The recovery and goal of strengthening also depend on the final goal to be achieved for the back pain patient. It takes a few weeks to return to normal life and a few months of monitored rehabilitation for people who need to return to sports or lifting weights pain-free in the gym.
When is surgery for severe cases of disc herniation required?
If the symptoms of back pain, weakness, numbness and referred radiating pain down the buttocks and thighs and legs continue, along with pre-existing spinal issues like stenosis or spondylitis continue, and if physical therapy and pain killers do not work, the option of surgery can be advised by the orthopaedic surgeon.
SUMMARY:
Discs are meant to take shear and compressive forces and strengthening the spinal muscles aid in the recovery of the weak muscles and improving spinal posture and health.
Proper loading in exercises helps the discs to adapt back into the spine without causing major recurring spinal symptoms.
~ Authored by Dr Janhvi Vayada (Sports Physiotherapist, Mind Your Fitness!)